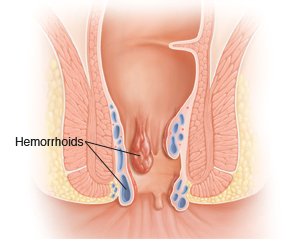
Hemorrhoids are swollen and inflamed veins inside the rectum and near the anus. The rectum is the last several inches of the colon. The anus is the passage between the rectum and the outside of the body.
Causes
The veins can become swollen because of increased pressure in them. This is most often caused by:
-
Long-term (chronic) constipation or diarrhea
-
Straining when having a bowel movement
-
Sitting too long on the toilet
-
A low-fiber diet
-
Pregnancy
-
Supporting tissues of the anus and rectum get weaker with aging or during childbirth
Symptoms
-
Bleeding from the rectum. You may notice this after bowel movements. If you see blood from bowel movements, talk with your healthcare provider. They can determine if it's likely to be hemorrhoids, or if you need more assessment.
-
Lump near the anus
-
Itching around the anus
-
Pain around the anus
-
Mucus leaks from the anus
There are different types of hemorrhoids. Depending on the type you have and the severity, you may be able to treat yourself at home. In some cases, certain procedures may be the best treatment choices. Your healthcare provider can tell you more about this if needed.
Home care
General care
-
To get relief from pain or itching, try:
-
Medicines. Your healthcare provider may recommend stool softeners, suppositories, or laxatives to help manage constipation. Use these exactly as directed.
-
Sitz baths. A sitz bath involves sitting in a few inches of warm water. Be careful not to make the water so hot that you burn yourself—test it before sitting in it. Soak for about 10 to 15 minutes a few times a day. This may help relieve pain.
-
Topical products. Your healthcare provider may prescribe or recommend creams, ointments, or pads that can be applied to the hemorrhoid. Use these exactly as directed.
-
Tips to help prevent hemorrhoids
-
Eat more fiber. Fiber adds bulk to stool and absorbs water as it moves through your colon. This makes stool softer and easier to pass.
-
Increase the fiber in your diet with more fiber-rich foods. These include fresh fruit, vegetables, and whole grains.
-
Take a fiber supplement or bulking agent, if advised by your healthcare provider. These include products such as psyllium or methylcellulose.
-
-
Drink more water. Your healthcare provider may direct you to drink plenty of water. This can help keep stool soft.
-
Be more active. Frequent exercise aids digestion and helps prevent constipation. It may also help make bowel movements more regular.
-
Don’t strain during bowel movements. This can make hemorrhoids more likely. Also, don’t sit on the toilet for long periods of time.
Follow-up care
Follow up with your healthcare provider as advised. If a culture or imaging tests were done, someone will let you know the results when they are ready. This may take a few days or longer. If your healthcare provider recommends a procedure for your hemorrhoids, these choices can be discussed. Choices may include surgery and outpatient office treatments.
When to get medical advice
Call your healthcare provider right away if any of these occur:
-
Increased bleeding from the rectum
-
Increased pain around the rectum or anus
-
Black, tarry stools
-
Weakness or dizziness
Call 911
Call
-
Trouble breathing or swallowing
-
Fainting or loss of consciousness
-
Unusually fast heart rate
-
Vomiting blood
-
Large amounts of blood in stool