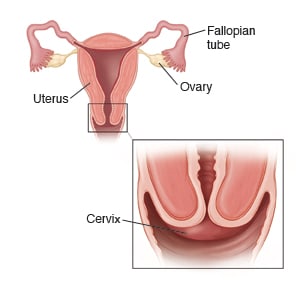
You have cervicitis. This is when the opening to the uterus (the cervix) becomes inflamed and irritated. It is often caused by an infection, and it needs to be treated.
What causes cervicitis?
Acute cervicitis is usually caused by an infection.
- The infection is often a sexually transmitted infection (STI). These are spread by having vaginal, anal, or oral sexual contact with someone who is infected.
- Chlamydia and gonorrhea are two common STIs that cause cervicitis. These STIs are very contagious. They can be spread during sex from an infected person until that person gets treatment.
- Other bacteria that can cause cervicitis include Mycoplasma genitalium, trichomonas, and herpes.
Sometimes the cause of cervicitis can't be identified.
What are the symptoms of cervicitis?
At first, cervicitis may cause no symptoms or only mild symptoms. When symptoms occur, they may come on quickly. The most common symptoms are:
- Vaginal discharge.
- Vaginal bleeding.
- Pelvic pain.
- Pain when urinating.
- Pain with intercourse.
Often there is no fever. If you have a fever, it may be a sign that the disease has spread to the fallopian tubes and caused pelvic inflammatory disease (PID).
After many days to a few weeks, these symptoms go away and you may have no symptoms at all. But the infection is still there and you can still spread it to others.
How is cervicitis treated?
Remember that cervicitis is often the result of a STI. If you have no symtpoms, you can give it or get it without knowing.
Whether or not you have symptoms, it is important to treat cervicitis. This is to prevent it from damaging the uterus, spreading to the fallopian tubes, and becoming PID. If not treated, chlamydia or gonorrhea can scar the uterus and fallopian tubes. Scarring can cause infertility (being unable to have children). PID also increases the risk of having a pregnancy outside the uterus (ectopic pregnancy) in the future.
This infection can be treated and cured. The infection is treated with antibiotic medicine.
To figure out the type of infection you have and decide on the best treatment, your doctor may do some tests, such as:
- Nucleic acid (DNA) testing for signs of the germs.
- Analysis of samples under a microscope.
- Cultures, which are samples of cells grown and observed in a lab.
DNA tests and cultures may take a few days to show results.
Home care
- Once your condition is diagnosed, your sexual partner should also be treated at the same time, even if there are no symptoms. Your partner should call their doctor. Or they can go to an urgent care clinic or the public health department to be examined and treated. In some cases, your doctor may give your partner a prescription for antibiotics. This is called expedited partner therapy.
- Don't have sex until both you and your partner have completed all antibiotic medicine and your doctor has told you that you are no longer contagious. This is often no sooner than 7 days after treatment.
- Take all medicines until they are gone. If not, the illness may recur.
- Learn about safer sex practices and use these in the future. The safest sex is with a partner who has tested negative and only has sex with you. Condoms can protect you from some STIs, including gonorrhea, chlamydia, and HIV. But they are not a guarantee. Taking medicines to prevent HIV may also be a good idea for you. Ask your doctor if you should start taking PEP (HIV post-exposure prophylaxis) or PrEP (HIV pre-exposure prophylaxis).
Follow-up care
Follow up with your doctor as advised.
- Only people who are pregnant need a follow-up test after treatment to see if they are cured.
- If a DNA test or culture was done, you will be told if the treatment needs to be changed. You can call as directed for the results.
- Follow up with your doctor or the public health department for complete STI screening, including HIV testing.
When to call for help
Call
- You have trouble breathing.
- You have chills or fever.
- You have abdominal pain.
- You have uncontrolled vaginal bleeding.
- You have extreme confusion.
- You have extreme drowsiness or trouble awakening.
- You have fainting or loss of consciousness.
- You have a rapid heart rate.
Contact your doctor now or seek immediate medical care if:
- You have no improvement after 3 days of treatment.
- You have new or increasing lower abdominal pain or back pain.
- You have vaginal bleeding between menstrual periods.
- You have weakness or dizziness.
- You have repeated vomiting.
- You are unable to urinate due to pain.
- You have a rash or joint pain.
- You have painful open sores around the outer vagina.
- You have enlarged, painful lymph nodes (lumps) in the groin.
- You have a fever of 100.4ºF (38ºC) or higher, or as directed by your doctor.

